Japanese art inspires personalized treatment model for glioma
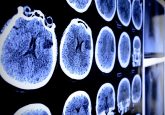
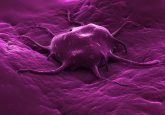
Researchers have developed ‘artificial mini brains’ – organoids – that could be used to develop personalized brain cancer treatments. The organoids, developed via on a technique inspired by the ancient Japanese art of flower arranging, consist of human neural stem cells printed onto a microneedle plate that grow into miniature 3D environments suitable for modeling tumor growth and treatment. These organoids provide an authentic model – the first of its kind – for modeling how brain tumors grow and respond to different treatments. The project was conceived by Christian Naus (University of British Columbia, Vancouver, Canada) with Japanese bioprinting company...